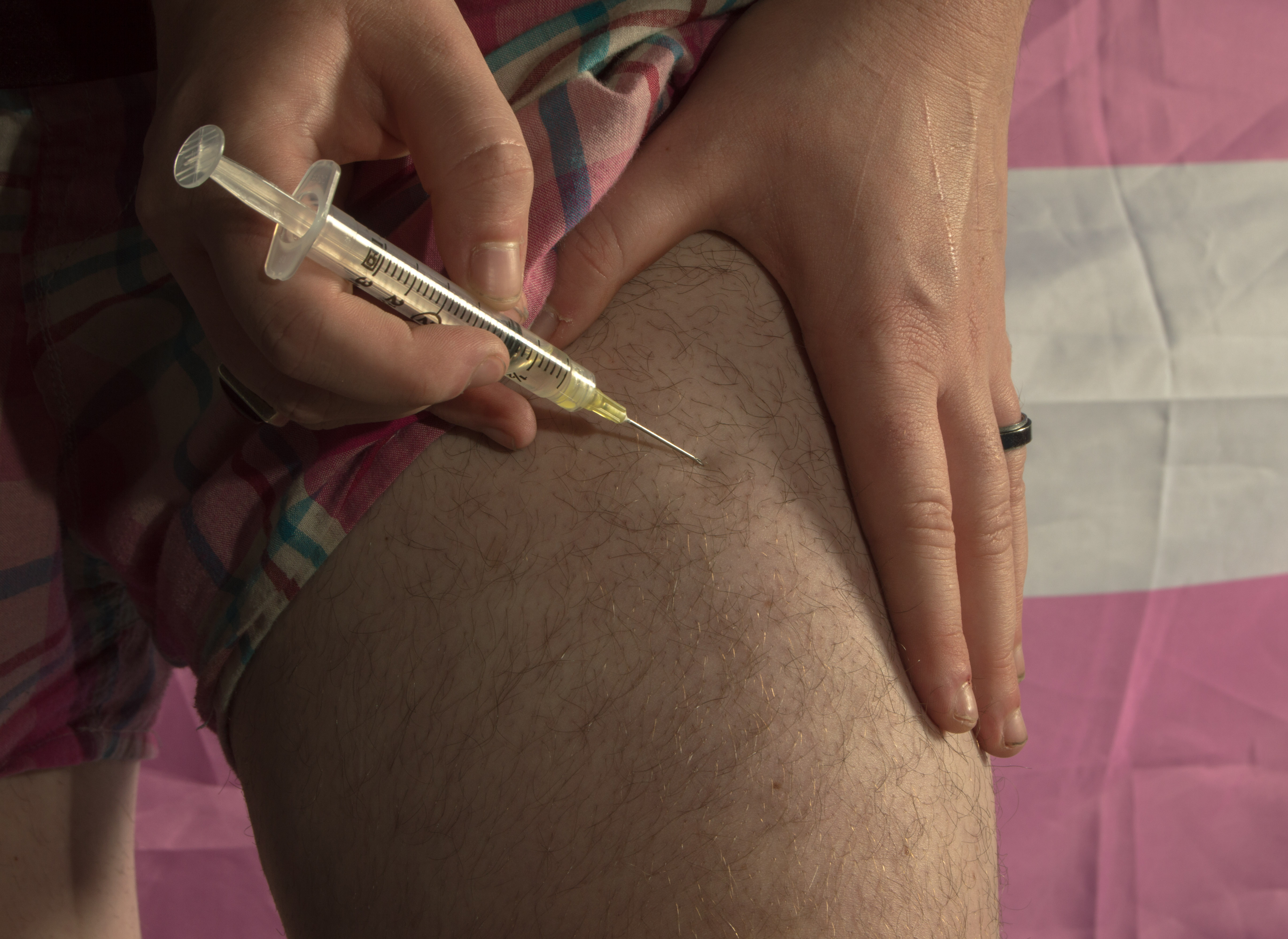
For those who are transgender, maintaining their health requires additional care cisgender people may not consider.
Jordan White was in high school when he first came out. He was in the car with his sister and had been debating whether he should tell her or not. His stomach churned and his hands were sweaty, but he finally worked up the courage to tell her.
“Brianna, I’m a lesbian.”
Brianna said, “I don’t give a shit. You can be whoever you want to be.” And without missing a beat, transitioned into talking about boy bands.
A few years later when he started college, Jordan came out to Brianna again. This time he told her he was transgender. He said he never really felt like a girl and would be transitioning to male. Again, Brianna was nonchalant about Jordan’s news and told him to be who we wanted to be.
Jordan is among the 1.4 million adults in the United States who identify as transgender. This is roughly 0.6 percent of the U.S. adult population.
Transgender individuals have additional health concerns that cisgender people—those who identify with their birth sex—don’t have to consider. These additional considerations affect different aspects of a person, including their physical, mental, and sexual health.
After coming out as transgender, Jordan started wearing a binder on his chest to hide his breasts. He cut his already-short hair even shorter. He started wearing baggy clothes from the men’s department to hide his curvy figure. He lowered his voice when he spoke. Jordan did everything he could to come off as male.
And on May 4, 2017 at 20 years old, Jordan finally injected his first hormone shot.
Like Jordan, 18-year-old Maxwell Ritchie injects testosterone into his thigh to help his transition from female to male.
Testosterone had been on the radar for Jordan since he first began to identify as male. He had been preparing for months before his procedure started, studying every piece of information he could get his hands on.
Jordan knew that he would need a thick plastic container to dispose of his used needles after each injection. In March, he set aside an empty Tide Pods container specifically for this.
Before Jordan could start taking testosterone, he had to obtain written approval from his therapist saying that he was of sound mind and able to appropriately make the decision. This is the process in Indiana, but in some other states patients are required to go through a series of physical tests in order to start testosterone treatment.
The written approval comes after a series of assessments. Dr. Erica Kane, a psychologist and owner of Kane Loveridge Wellness Group in New Castle, Indiana, says these assessments evaluate dysphoria through psychosocial adjustment. Psychologists assess their patients’ gender identities related to their dysphoria and the history and development of the dysphoria. They also explain the stigmas behind gender non-conformity, discuss patients’ emotional support, and make sure the patients are mentally stable before starting hormone therapy.
Dr. Kane wants to make sure her patients are strongly rooted in their identities before moving forward in a process that may not be reversible.
After being assessed, individuals who identify as transgender are able to go to a medical provider to start the physical part of their treatment. While psychologists explain the mental health involved in transitioning with their patients, medical providers go over the physical side effects.
People are able to take testosterone in different forms: injection, gel, skin patch or a pill. Jordan chose injection because he doesn’t trust the other options. According to a hormone guide for female-to-male transitions from Carleton College, the pill is the least effective in stopping menstrual periods. One pump of gel is supposed to equal one 10-milligram dose of testosterone, but it’s hard to measure to make sure its user is being administered a proper dosage.
In addition to taking hormones, Jordan plans to get a double mastectomy to remove his breasts. This is one surgical option for female-to-male transitions, often referred to as “top surgery.” There are two common options for its counterpart, “bottom surgery,” or genital reconstruction surgery. Phalloplasty involves creating a prosthetic penis, while metoidioplasty involves administering testosterone to enlarge the clitoris, and uses surrounding skin to form a penis, according to FTM Surgery Network. But research and technology surrounding both are not at a level that Jordan trusts.
He has no interest in undergoing genital reconstruction surgery. He believes the testosterone and the double mastectomy will be enough to stifle his dysphoria and make him feel more comfortable with himself.
The average cost for a person to undergo both a double mastectomy and genital reconstruction surgery is $17,900. Testosterone injections are typically the cheapest option for hormonal therapy, ranging from $40 to $200 a month, according to Scottsdale Restorative Medicine.
Under the Affordable Care Act (ACA), most insurers can’t limit or deny coverage simply because someone needs treatment related to their gender identity. This regulation only applies to programs that receive federal funding, administered by a federal agency, or governed by any entity established under Title I of the ACA.
Health insurance companies cannot limit services based on a person’s sex assigned at birth. For example, a transgender man is covered to receive a mammogram or a Pap smear. However, many health plans still use exclusions such as “services related to sex change” or “sex reassignment surgery” to deny coverage to transgender people for certain health care services, according to healthcare.gov.
For those whose insurance does not cover these surgeries, or those who have not yet undergone the procedure, day-to-day life can take a toll on their mental well-being.
Jordan wears a binder throughout the day to hide his chest, but he doesn’t wear one to bed. So, when he wakes up in the morning, Jordan doesn’t have to force the tight fabric off his chest before getting in the shower. That doesn’t mean that his shower routine is without complications, however.
Jordan doesn’t look in the mirror before showering. He knows that if he catches a glimpse of his naked body that doesn’t match his gender, he won’t be able to stop the tears spilling from his eyes.
He quickly gets in the shower. Afterward, he wraps his towel around himself before pushing the shower curtain aside. Jordan quickly scoops up his clothes from the floor and heads back to his room to get dressed, never once looking at the bathroom mirror.
Some days he is successful in avoiding his reflection. But when he does happen to see himself, the dysphoria takes over and sends his mental health into a whirlwind.
Gender dysphoria is the feeling of stress, anxiety, and restlessness caused by someone’s physical body not matching up with his or her gender identity, according to the American Psychiatric Association. Jordan describes dysphoria as the lovechild of depression and anxiety. When someone misgenders Jordan, he experiences extreme dysphoria. He collapses into himself to hide his figure and his breath shortens as if he were having a panic attack.
Jordan was in The Container Store in Indianapolis shopping for storage bins with Brianna, who needed the bins for her apartment. The day started out as a sibling bonding day, the brother and sister enjoying their time together. They laughed and made jokes with and about each other. The two are close, but do not get to hang out as often as they’d like because they live in different cities.
After finding bins the right size for Brianna’s apartment, the two headed toward the long check-out line. To pass the time, an older woman in front of them was making small talk with other people in line. To Jordan, the woman looked like a “minivan mom” with her short hair and plain, frumpy clothes. She looked past Jordan and asked some women behind him about their shopping habits.
After chatting for a few minutes, she turned to Jordan and his sister and asked, “Out of you ladies, who’s the shopper?” Jordan cringed. This wasn’t the first awkward interaction that Jordan had encountered during his two years as a transgender man.
Brianna answered for both of them, so Jordan wouldn’t have to. She casually played it off by appointing herself the shopper of the two.
As he reflected on the seemingly-innocent question, hateful thoughts flooded Jordan’s head. What gave it away? My princess shoes? Did I talk too much? Did I cock my hip?
The “minivan mom” couldn’t have known she would trigger Jordan’s internal identity crisis. To her, she was simply asking two young women about their shopping preferences. After Brianna answered, the woman seemed satisfied and turned back around.
Even with all of Jordan’s efforts—binding his chest, lowering his voice, and taking on every stereotypically-male quality he can—people like the woman in The Container Store still perceive him as female. This is when Jordan experiences debilitating dysphoria.
Being addressed as a woman hurts Jordan’s emerging view of himself as a man. He feels as if he is dragged back into his past self every time he is called “ma’am” or “miss” or “lady.” That’s not who he is, but it’s still how many other people see him.
His mom, aunts, and grandma slip up sometimes and call Jordan “she” or “her.” He knows it’s difficult for them. But, he still corrects them when they mess up. The only exception Jordan makes for being addressed as female is with his father. Jordan’s dad outright told Jordan he could not address him as a male. He told Jordan, “You’re my little girl and that’s how I’ll always see you.”
Dr. Kane says this may bother some individuals, but others, like Jordan, can put their feelings on hold to maintain relationships. Because pronouns correlate with a person’s identity, Dr. Kane says making exceptions like this is individual and can vary by person.
The stigmas and lack of support regarding transgender people lead to higher rates of suicide and depression, Dr. Kane says. According to the Williams Institute, 41 percent of transgender individuals attempt suicide, compared to the 4.6 percent of the overall U.S. population who report lifetime suicide attempt.
Many people who identify as transgender experience dysphoria their whole lives, Dr. Kane says. They don’t feel like they’re living a life they were meant to live.
Because Jordan is not yet 21, he has not been required to get a Pap smear. The thought of going to the gynecologist is terrifying for him. LGBT clinics help find doctors who are up to date on transgender health, but Jordan still can’t imagine going to a gynecologist appointment while on testosterone and looking like a man. He gets anxious thinking about all the dirty looks he presumes he’ll receive.
This is an area in which Dr. Kane is trying to raise awareness. If an individual presents as a man and walks into an appointment requesting a Pap smear, they may receive confused responses from health professionals. Dr. Kane says it’s not that these professionals are trying to be insensitive, they just don’t have the education they need to interact with transgender patients.
Though it may be uncomfortable, it’s necessary for transgender individuals to keep up with their sexual health. Transgender people face high risk for HIV infection, and even though a person may identify differently from their birth sex, they still have to consider the health possibilities that correlate to that sex.